
Pelvic pain and sexual dysfunction
June 19, 2025
Physiotherapy after Breast Cancer
June 19, 2025What is it and could I have one?
Figures suggest that 1 in 3 women experience Pelvic Organ Prolapse (POP). 50% of women who give birth will have a prolapse. 50% of women over the age of 50 will have some symptoms of prolapse. These are pretty significant and scary numbers for women but don’t worry!
Pelvic organ prolapse is a common health issue. It’s important to know that it can be managed and even prevented with the right treatment. There are many ways of treating prolapse that do not involve medication or surgery.
Pelvic floor physiotherapy combined with some simple changes to your daily habits may help reduce your symptoms.
So what is a prolapse?
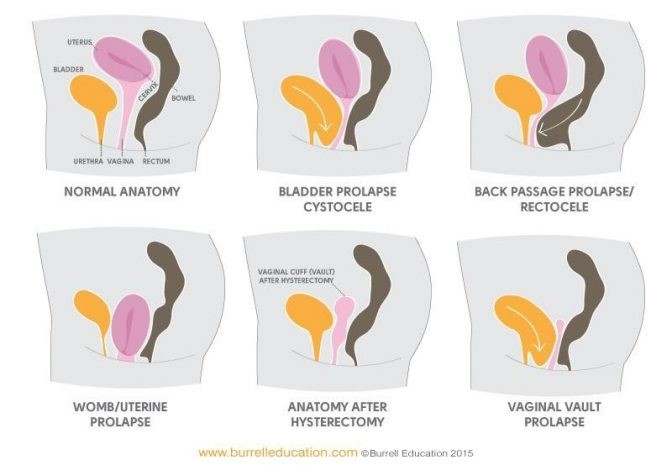
A Pelvic Organ Prolapse (POP) occurs when a pelvic organ or organs bulge into the vagina. It can be due to weakened, damaged or strained ligaments, muscles or fascia of the pelvis. There are different types of prolapse depending on which organ (bladder, rectum or uterus) is bulging into the vagina. You can have more than one prolapse at the same time.
A cystocele is when the bladder drops down into the anterior aspect of the vagina, a rectocele is when the rectum drops down in the posterior aspect of the vagina, a uterine prolapse is when the womb descends and a vaginal vault prolapse is when post hysterectomy the vagina drops downwards.
Some common risk factors/causes of Pelvic Organ Prolapse include:
- Pregnancy and childbirth (main cause) – 50% of women who have had a vaginal delivery will have a prolapse. Pregnancy hormones and weight gain also have an impact on the pelvic structures.
- Chronic coughing from smoking or respiratory disorder increases downward pressure.
- Constipation and chronic straining to defaecate stresses the pelvic floor.
- Heavy lifting – poor technique and holding our breath during exercising can increase intra-abdominal pressure.
- Obesity increases pressure on the pelvic structures.
- Age – transition through the menopause can trigger prolapse symptoms due to the hormonal and tissue changes (often the weakness was always there but highlighted during/after menopause)
- Following hysterectomy when ligamentous and fascial support has changed or may be removed.
What are the symptoms of prolapse?
You may not even know you have a prolapse as there may be no symptoms early on. Also, signs will differ depending on the type of prolapse you have. Symptoms generally can be more noticeable towards the end of the day, after prolonged standing or with straining. Symptoms may include
- Pelvic pressure – often described as a dragging/ heaviness/ lump in the vagina. Some report sensations of “sitting on an egg” or feeling of something “falling out”. At times you may feel/see a bulge.
- Urinary symptoms – leakage (dribble after standing up), increased frequency, difficulty emptying or slow flow of urine, frequent urinary infections.
- Bowel symptoms – pain, pressure, constipation.
- Sexual problems with pain and/or sensation
- Low back pain/Abdominal pain (usually temporary)

What is the treatment?
The earlier we can get started on treatment for prolapse the more successful the outcome can be. Prolapse can have different emotional and physical impact on every woman with different appearance, limitations and symptoms. There is good news however, as research shows that pelvic floor physiotherapy, and simple changes to your daily habits, can help manage and improve your symptoms.
A first step in the right direction is to seek out the help and treatment from a trained pelvic health physiotherapist.
Treatments may consist of pelvic floor muscle training, learning the knack to help brace against increased intra-abdominal pressure, abdominal exercises, breathing and postural advise +/-correction, lifestyle changes, advise on pelvic floor safe exercising, management tips, correct position for defecation and finally good bladder and bowel habits.
A pessary may be suggested to help manage symptoms. This is a device inserted into the vagina to help support the structures.
Surgery is an option if conservative treatments are not adequately helping and the prolapse is severe and/or affecting your quality of life.
 Where to get help?
Where to get help?
Unfortunately, Pelvic Organ Prolapse will not go away on its own. Worryingly, if you do nothing your symptoms may get worse. Please don’t ignore the signs and symptoms.
Research has shown that three months of pelvic floor muscle training with the guidance of a pelvic health physiotherapist can treat certain prolapses without the need for surgery. Symptoms can be improved.
Investing in your pelvic health is worth it
If you are having any issues with signs and symptoms of prolapse or think you are at risk please call for an appointment with Sylvia Farrell our Pelvic Health Specialist.

Appointments
Sylvia is available for appointments on, Tuesdays, Wednesdays, Thursdays and Fridays. If you would like to book a session with Sylvia you can call the clinic on 091 727777 or get in touch via the contact page.




